If you have struggled your whole life with painful, heavy legs that don’t respond to diet or exercise, you are not alone. And you may not be dealing with a weight problem at all.
Lipedema is a chronic medical condition that causes an abnormal buildup of fat in the limbs, primarily the hips, thighs, and legs. It affects an estimated 5 to 12% of women in the United States, potentially 10 to 17 million people, yet it is widely underdiagnosed. Many women spend years, even decades, being told to “just lose weight” before they ever receive an accurate diagnosis.
Dr. Thomas Wright has been treating patients with lipedema for more than 20 years. He was recently featured in a Q&A with Vein Health News, a clinical publication for healthcare providers, as part of their comprehensive issue on lipedema. We’re sharing the key insights from that issue here, because every woman with lipedema deserves to be heard, believed, and properly cared for.
What Is Lipedema?
Lipedema is a loose connective tissue disorder that causes fat cells to accumulate abnormally in the limbs. Unlike typical body fat, lipedema fat is:
- Located primarily in the hips, thighs, legs, and sometimes arms, not distributed throughout the whole body
- Symmetrical, affecting both sides equally
- Typically sparing the hands and feet, sometimes creating a distinctive “cuff” at the wrists or ankles
- Resistant to diet, exercise, and even bariatric surgery
The fat tissue in lipedema can feel unusual, lumpy, nodular, or fibrous, sometimes described as feeling like rice, peas, or walnuts beneath the skin. This is very different from typical subcutaneous fat.
The cause of lipedema is not fully understood, though it is believed to be hereditary and related to hormonal factors. It occurs almost exclusively in women, and symptoms often emerge or worsen during hormonal changes like puberty, pregnancy, or perimenopause.

Lipedema Is Not Obesity, And It’s Not Your Fault
One of the most damaging misunderstandings about lipedema is that it results from poor lifestyle choices. It does not. Lipedema is a medical condition, one that happens to involve fat tissue, but is fundamentally different from general obesity.
While obesity-related fat occurs throughout the body and is generally responsive to calorie reduction, lipedema fat accumulates in specific areas and resists conventional weight loss efforts. Many women with lipedema maintain a healthy weight in their upper bodies while experiencing significant enlargement in their lower extremities.
Lipedema is also distinct from lymphedema, a condition caused by lymphatic fluid buildup. The two can co-occur, a combined condition called lipo-lymphedema, but they have different causes and require different treatment approaches.
Lipedema is frequently mistaken for both obesity and lymphedema, and diagnosis is often delayed as a result.
Recognizing the Symptoms of Lipedema
Lipedema symptoms can vary from person to person and often worsen over time, particularly during hormonal changes. Common signs include:
- Disproportionately large hips, thighs, and legs compared to the upper body
- Pain, tenderness, or sensitivity to touch in the affected areas
- A feeling of heaviness or fatigue in the legs
- Easy bruising in the legs or arms
- Swelling that worsens throughout the day or with prolonged standing
- A lumpy or nodular texture beneath the skin
- Legs or arms that do not change significantly with diet or exercise
- A “cuff” of fat at the ankles or wrists, with the hands and feet relatively unaffected
If several of these symptoms sound familiar, it may be worth speaking with a lipedema specialist. Diagnosis is clinical, there is no blood test that can confirm lipedema, so it requires a physician who knows what to look for.
How Lipedema Is Diagnosed
Because there are no definitive biomarkers for lipedema, diagnosis depends on a thorough patient history, physical examination, and ruling out other conditions. A knowledgeable clinician will assess:
- Whether fat is distributed symmetrically and disproportionately in the limbs
- Family history of similar body shape patterns
- Whether symptoms began or worsened during hormonal changes
- Whether fat tissue is resistant to dietary intervention and exercise
- The presence of pain, tenderness, or easy bruising in the affected areas
- Whether the hands and feet are spared
Lipedema is also classified by type (based on location of fat deposits) and by stage (based on severity). The staging system helps guide treatment decisions, from conservative management to surgical intervention.
The U.S. Standard of Care Committee published consensus guidelines for lipedema diagnosis in 2021 (1), helping to standardize how the condition is evaluated and treated across the country.
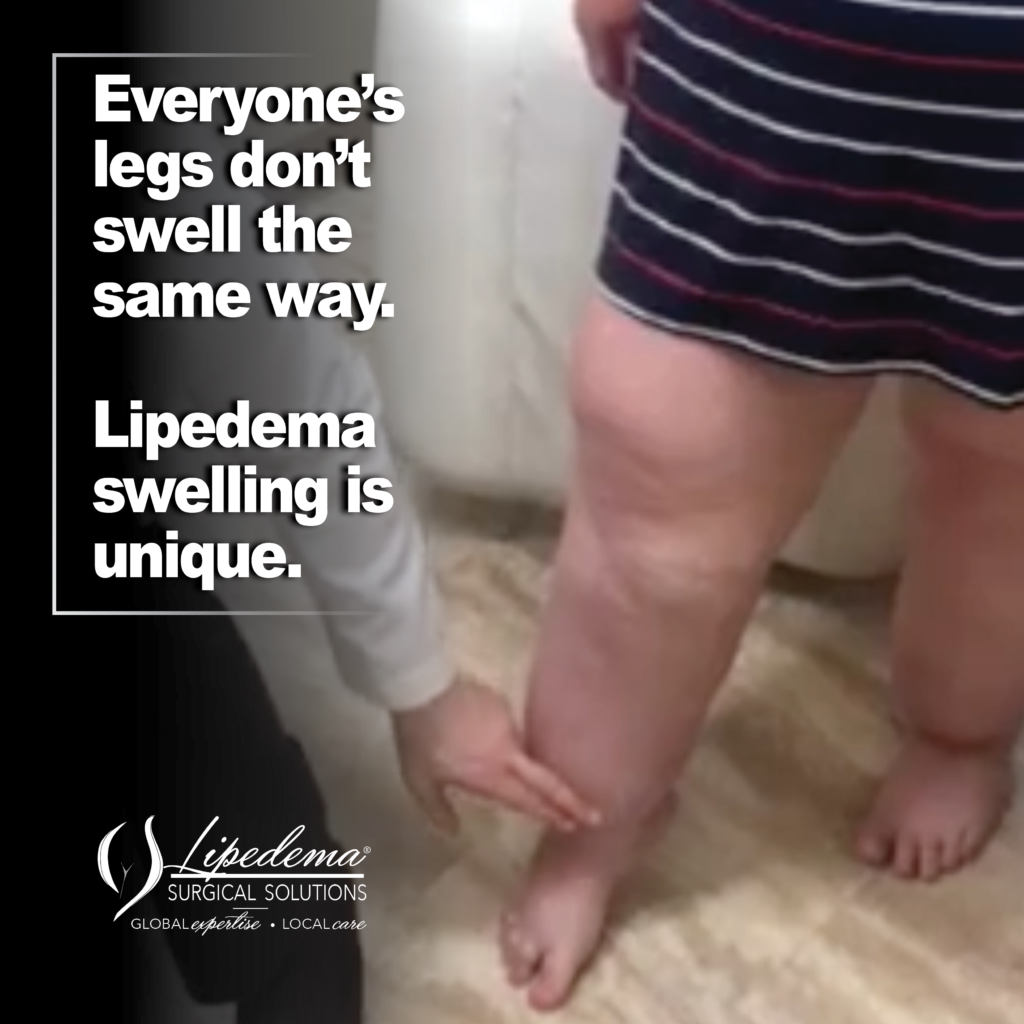
Treatment Options: A Comprehensive Approach
While there is currently no cure for lipedema, there are meaningful ways to manage symptoms and improve quality of life. Treatment works best when it is comprehensive, addressing the condition from multiple angles at once.
Diet and Nutrition
An anti-inflammatory diet is one of the most important tools for managing lipedema. Approaches that limit refined carbohydrates, such as ketogenic, low-carbohydrate, or Mediterranean-style diets, can help reduce swelling and inflammation. Diet won’t eliminate lipedema fat, but it can help slow progression and reduce the factors that make symptoms worse.
Medical-Grade Compression
Graduated compression therapy is considered a first-line treatment for lipedema. Worn daily, compression garments can reduce pain, improve mobility, decrease swelling, and support lymphatic function. Dr. Wright emphasizes that compression is foundational, both as a standalone treatment and as essential preparation for surgery.
Manual Lymphatic Drainage (MLD)
MLD is a gentle, specialized massage technique performed by a Certified Lymphedema Therapist. It helps move fluid out of affected tissues and can slow the progression of lipedema. Many patients are also taught self-massage techniques to support their daily management at home.
Exercise
Low-impact movement is important for lymphatic health and overall well-being. Water aerobics, swimming, walking, yoga, and Pilates are particularly well-suited for patients with lipedema, they support lymphatic drainage without placing excess stress on painful joints.
Medications
Certain medications may help reduce inflammation and manage symptoms. GLP-1 and GIP agonist medications, such as semaglutide and tirzepatide, have shown potential to reduce pain and inflammation in some lipedema patients, even before significant weight loss occurs. Dr. Wright offers these medications through Wright Choice Weight Loss as part of a comprehensive care plan. Other options may include Metformin for patients with metabolic comorbidities and anti-inflammatory supplements such as turmeric or Diosmin MPFF.
Lipedema Reduction Surgery
For patients whose symptoms are not adequately managed through conservative treatments, lipedema reduction surgery, a specialized form of liposuction, can provide significant relief. Dr. Wright is one of the most experienced lipedema surgeons in Missouri, with over 20 years of specialized practice and published outcomes data.
The landmark LIPLEG study, a randomized controlled trial, found that more than 70% of women who underwent lipedema liposuction experienced significant improvement in pain and quality of life, compared to just 10% in the conservative treatment group. The study showed a 26:1 odds ratio of significant improvement for those who had surgery.
Surgery is not a cure, but it can meaningfully reduce lipedema tissue, improve mobility, decrease pain, and in many cases halt disease progression.
The Emotional Side of Lipedema
Living with lipedema can take a profound emotional toll. Many women have spent years being dismissed by doctors, blamed for a condition they did not cause, and told that if they just tried harder, their legs would look different.
That kind of repeated dismissal can lead to depression, anxiety, low self-esteem, and disordered eating. Research confirms there is a higher prevalence of depression and other mental health conditions among people with lipedema.
If you have experienced this, please know: it was not your fault. You deserved to be listened to, and you deserve proper care now.
Emotional support, whether through counseling, patient advocacy groups, or online communities, is an important part of a complete lipedema treatment plan. Many patients find connection with others who share their experience to be enormously healing.
Read More: Vein Health News Lipedema Issue
Dr. Wright was recently featured in a detailed Q&A in Vein Health News, a trusted publication for primary care physicians and healthcare providers. The issue covers everything from how lipedema is diagnosed to the role of surgery, compression, and emotional support, and it’s available free to the public. We encourage you to read it for a deeper understanding of this complex condition.
Getting Lipedema Care in St. Louis and O’Fallon, Missouri
If you recognize yourself in the symptoms described here, you don’t have to keep searching for answers alone. Dr. Thomas Wright and the team at Laser Lipo and Vein Center bring over two decades of specialized lipedema experience to patients across Missouri and the Midwest.
Dr. Wright offers a comprehensive approach to lipedema care, from conservative management with compression, diet, and GLP-1 medications, to advanced lipedema reduction surgery for appropriate candidates. He has published outcomes data from his practice and is recognized by organizations including the National Lymphedema Network and AVLS Congress for his contributions to the field.
You deserve to feel better. Reach out today to schedule a consultation and take the first step toward real answers.
Sources
- Herbst KL, Kahn LA, Iker E, et al. Standard of care for lipedema in the United States. Phlebology. 2021;36(10):779-796. Vein Health News, Volume 10 Issue 1. veinhealthnews.com LIPLEG Study: lipedema.net/groundbreaking-lipleg-study-results-transform-lipedema-treatment-germany-leads-the-way-in-evidence-based-care/