For years, women with lipedema are told the same things.
“You just need to lose weight.”
“Your legs are heavy because you’re out of shape.”
“Try compression and see how you feel.”
By the time most patients walk into a specialist’s office in Missouri, they have spent a decade or longer being dismissed by clinicians who confused their condition with obesity.
Lipedema is not obesity. It is not poor discipline. It is a chronic, progressive disorder of the subcutaneous fat that affects an estimated 11 percent of women, according to commonly cited figures in the lipedema research community. For many patients, conservative care helps manage symptoms but cannot stop the disease from progressing. That is where lipedema reduction surgery becomes a turning point.
What is Lipedema?
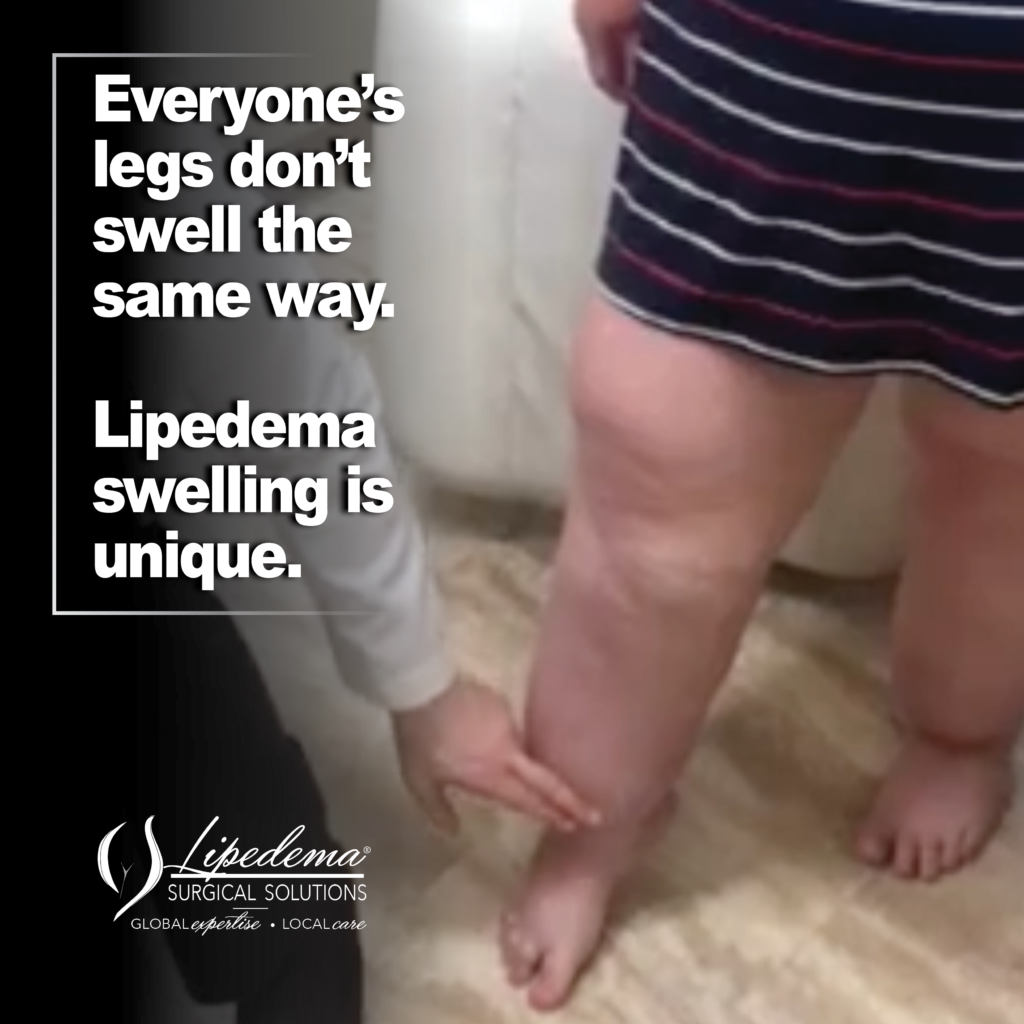
Lipedema is a disorder of fat distribution. It causes a symmetrical, disproportionate buildup of fat on the legs, hips, buttocks, and often the arms, while sparing the hands and feet. The classic visual sign is the “cuff” at the ankle or wrist, where the affected fat stops abruptly.
But the visible shape is only part of the picture. Lipedema fat is structurally different from ordinary fat. It contains fibrotic nodules, increased fluid in the surrounding tissue, and inflammation that produces real, measurable pain.
The Symptoms No One Talks About
When patients describe their lipedema to friends or unfamiliar doctors, they tend to focus on appearance because that is what shows. The symptoms that affect daily life are harder to articulate.
- Pain and tenderness in the affected limbs, often worse with prolonged standing
- Easy bruising with no clear cause
- A feeling of heaviness or fatigue in the legs by mid-afternoon
- Fibrotic nodules that feel like small pebbles or rice grains under the skin
- Reduced mobility as fat volume increases at the knees and inner thighs
- Skin changes including a cool, doughy texture
- Mental health impact from years of being misdiagnosed and dismissed
These are not cosmetic complaints. They are the symptoms of a connective tissue and lymphatic disorder, and they tend to worsen over time without intervention.
Why Conservative Treatments Often Aren’t Enough
Compression garments, manual lymphatic drainage, anti-inflammatory eating patterns, and low-impact exercise all play important roles in lipedema care. They reduce fluid, ease discomfort, and slow progression for many patients.
What they cannot do is remove the diseased fat that is already there.
This is where so many patients hit a wall. They follow every recommendation. They wear the compression. They go to therapy. And the lipedema fat continues to accumulate because the underlying tissue is not responding the way ordinary fat would. Diet and exercise can help maintain overall health and reduce non-lipedema fat, but the lipedema-specific tissue is largely resistant to those efforts.
How Lipedema Reduction Surgery Helps
Lipedema reduction surgery uses lymph-sparing tumescent liposuction techniques, most commonly power-assisted liposuction (PAL) or water-assisted liposuction (WAL), to remove the diseased fat while protecting the lymphatic vessels that run through it.
This is fundamentally different from cosmetic liposuction. The goals are functional:
- Reduce pain and tenderness
- Restore mobility and range of motion
- Slow or halt disease progression
- Improve the effectiveness of conservative care going forward
Long-term outcome studies, including the work of Baumgartner and colleagues following lipedema patients for up to 12 years after surgery, have documented sustained improvements in pain, bruising, and quality of life. The German LIPLEG randomized controlled trial added further evidence that liposuction provides meaningful symptom relief beyond conservative therapy alone. Further evidence showed the odds of significant relief was 26x more likely with lipedema reduction surgery combined with conservative treatment, compared to just conservative treatment alone.
What “Surgery as a Turning Point” Looks Like
Patients describe the change in different ways. Some say they could finally cross their legs. Others say they slept through the night for the first time in years because the chronic ache in their thighs had eased.
The shift is not always dramatic in the first week or two. Swelling needs time to resolve, and the body needs time to adjust. But by three to six months after surgery, most patients are noticing changes in how they move, how they feel at the end of the day, and how their clothes fit over the affected areas.
For patients with multiple stages of lipedema or involvement across multiple body areas, a series of staged procedures is often planned over the course of a year or more.
Who Should Consider Lipedema Reduction Surgery
Surgery is most often recommended for patients who:
- Have a confirmed diagnosis of lipedema
- Have tried conservative care and are still experiencing pain, mobility limits, or progression
- Are in good general health and a stable weight range
- Have realistic expectations about what surgery can and cannot do
A specialist consultation is the right place to map out whether surgery makes sense, which body areas to address first, and what the recovery and follow-up plan should look like.